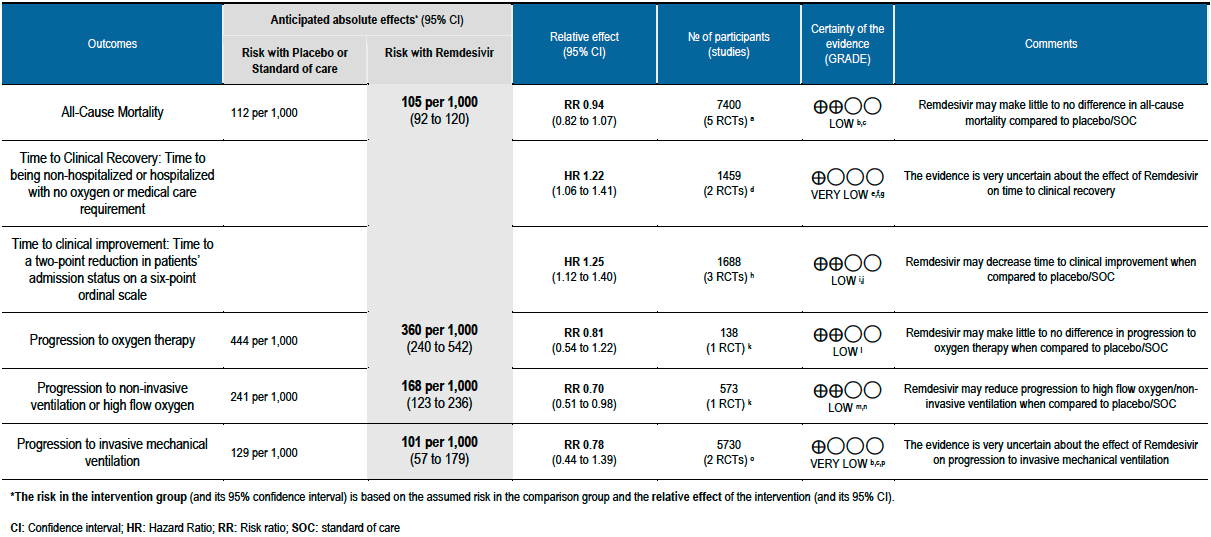
Summary of Findings Table 1 - Efficacy Outcomes:
GRADE Working Group grades of evidence
High certainty: We are very confident that the true effect lies close to that of the estimate of the effect
Moderate certainty: We are moderately confident in the effect estimate: The true effect is likely to be close to the estimate of the effect, but there is a possibility that it is substantially different
Low certainty: Our confidence in the effect estimate is limited: The true effect may be substantially different from the estimate of the effect
Very low certainty: We have very little confidence in the effect estimate: The true effect is likely to be substantially different from the estimate of effect
Explanations:
a. Wang 2020, ACTT Beigel 2020, Spinner 2020, Solidarity 2021, Mahajan 2021
b. Downgraded by one for level serious indirectness; The usage of steroids varied across the studies
c. Downgraded by one level for serious imprecision; the 95% CI is wide
d. ACTT Beigel 2020, Spinner 2020. Pooled estimate is from 2 trials at 10 days
e. Downgraded by one level for serious risk of bias; Spinner 2020 was at high risk of bias and contributed to 36.1% of the weight in the metanalysis
f. Downgraded by one level for serious indirectness; Spinner 2020 had moderate severity patients only and ACTT Beigel 2020 had a mixture of patients of different severity.
g. Downgraded by two levels for very serious imprecision; It is difficult to determine the clinical significance of the difference in the time to clinical improvement with hazard ratios, but the 95% CI was wide and included no difference.
h. Wang 2020, ACTT Beigel 2020 , Spinner 2020. Pooled estimate from 3 trials at 10 days
i. Downgraded by one level for serious risk of bias ; Spinner 2020 was at high risk of bias and contributed 25.9% of the weight to the pooled effect estimate.
j. Downgraded by one level for serious indirectness; The three studies included patients with different grades of disease severity and Spinner 2020 included only patients with moderate severity.
k. ACTT Beigel 2020
l. Downgraded by two levels for imprecision; 95% CI is very wide
m. Downgraded by one level serious indirectness; as very few people in ACTT Beigel 2020 were given steriods
n. Downgraded by one level for serious imprecision.The data were from only one trial and the number of events were too few to satisfy the requirements for the optimal information size (OIS) [The OIS for a RRR of 2 percent needs at least 700 events for the intervention to be significant (Remdesivir arm: 52/307, placebo arm: 64/266)]. The 95% CI of the effect estimate included clinically important and potentially clinically non-appreciable benefits with Remdesivir.
o. ACTT Beigel 2020, Solidarity 2021
p. Downgraded by two levels for very serious inconsistency; the I2 is 91%.
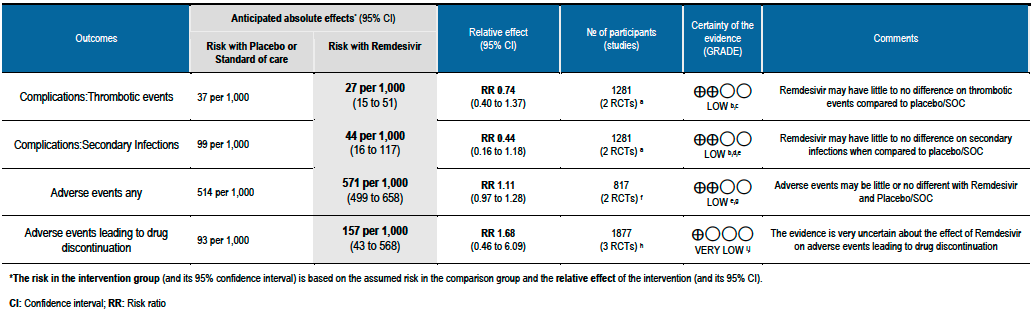
Summary of Findings Table 2 - Complications & Safety Outcomes:
GRADE Working Group grades of evidence
High certainty: We are very confident that the true effect lies close to that of the estimate of the effect
Moderate certainty: We are moderately confident in the effect estimate: The true effect is likely to be close to the estimate of the effect, but there is a possibility that it is substantially different
Low certainty: Our confidence in the effect estimate is limited: The true effect may be substantially different from the estimate of the effect
Very low certainty: We have very little confidence in the effect estimate: The true effect is likely to be substantially different from the estimate of effect
Explanations:
a. ACTT Beigel 2020, Wang 2020
b. Not downgraded for indirectness: Wang 2020 and ACCT Beigel 2020 included similar proportions of patients with severe disease and the incidence of adverse events was unlikely to have been confounded by severity.
c. Downgraded by two levels for very serious imprecision; the number of events were few and the 95% CI of the effect estimate included clinically important reductions and increases in thrombotic events with Remdesivir.
d. Downgraded by one level for serious inconsistency; the I2 is 65%
e. Downgraded by one level for serious imprecision: The number of events were few and the 95% CI of the effect estimate included a substantial reduction as well as a modest increase in the incidence of infections with Remdesivir compared to placebo/SOC.
f. Wang 2020, Spinner 2020
g. Downgraded by one level for serious risk of bias; Spinner 2020 was judged to be at high risk of bias and contributed 56.5 % of weight in the metanalysis
h. ACTT Beigel 2020 , Wang 2020, Spinner 2020
i. Downgraded by one level serious inconsistency; as I2 is 76%
j. Downgraded by two levels very serious imprecision; the 95% CI is very wide
Remdesivir is a monophosphoramidate adenosine analogue prodrug which is metabolized to an active triphosphate form that inhibits viral RNA synthesis via RNA dependent RNA polymerase [1]. It was developed as a therapeutic agent for treating RNA-based viruses such as Ebola virus, MERS, SARS-CoV-1 and other zoonotic coronaviruses [2]. It has demonstrated in vitro and in vivo antiviral activity against SARS-CoV-2 [3].
Remdesivir is widely used across the world and a number of guidelines have recommended its use in severe COVID-19 patients [4;5]. The recent WHO living guideline provides a conditional recommendation against the usage of Remdesivir in COVID-19 irrespective of the severity of the disease [6].
Since Remdesivir is currently the only antiviral drug recommended for severe COVID-19 by the Ministry of Health & Family Welfare guidelines, and appears to have a relatively good safety profile, it has been in high demand. Its current limited availability in India has led to a crisis involving desperate crowds flouting Covid-19 restrictions to avail the drug.
This review aims to provide a summary of the available evidence from randomized clinical trials of Remdesivir for treatment of acute COVID-19, for any duration, which could guide clinicians and researchers regarding the appropriate use of this drug in the future.
We searched the Cochrane Central Register of Controlled Trials (CENTRAL), Epistemonikos, and the COVID‐19‐specific resource www.covid‐nma.com, for studies of any publication status and in any language. We also reviewed reference lists of systematic reviews and included studies. We performed all searches up to 15 April 2021.
We included randomized controlled trials (RCTs) testing Remdesivir in people with COVID‐19, and extracted data for the following pre-defined outcomes:
- Critical (primary for this review):
- Mortality (all-cause): at 28-30 days, or in-hospital
- Progression to:
- Oxygen therapy
- Ventilation: non-invasive or invasive
- Critical/Intensive care (any reason) - Time to clinical improvement
- Time to clinical recovery
- Adverse events: all and serious
- Important (secondary):
- Time to negative PCR for SARS-CoV-2
- Duration of hospitalization
- Complications of COVID-19:
- Thrombotic events
- Pulmonary function/fibrosis
- Long COVID/post-acute sequelae COVID
- Secondary infections
Two reviewers independently assessed eligibility of search results. One reviewer extracted data from each included study, and assessed risk of bias using the Cochrane Risk of bias (RoB) v2.0 tool. Data and RoB assessments were checked by the second reviewer. The entire RoB assessment was scrutinized by the whole team for this review, to reach consensus.
We used RevMan 5.4 to perform meta‐analysis using a random‐effects model for outcomes where pooling of effect estimates was appropriate. We used risk ratios (RR) for dichotomous outcomes and hazard ratios for continuous outcomes, with 95% confidence intervals (CIs). We performed a subgroup analysis to explore the effect on mortality stratified by different oxygen and ventilation requirements at baseline.
We used the I2 statistic to measure residual heterogeneity. We used GRADE methodology to assess the certainty in the evidence, and documented this in a ‘Summary of findings’ table using GradeProGDT.
We included five trials involving 7452 participants, all of whom were adults, and 3886 of whom received Remdesivir [7-11]. Two trials reported each from a single country: China [7] and India [10]; two from multiple countries in North America, Europe and Asia [8;11]; one recruited worldwide [9]. All trials were done in hospitalized patients. Disease severity, prevalence of comorbidities, and use of co‐interventions varied substantially between trials. Out of the five trials three [7;9;11] were found to have low risk of bias across all domains for all outcomes and two [8;10] had high risk of bias across multiple domains. Risk of bias for each domain per trial is displayed alongside the forest plots below.
The following comparisons were investigated in the trials (we compared outcomes for arms randomized to Remdesivir vs. outcomes for arms randomized to standard of care or placebo):
- Two trials [7;11] compared Remdesivir with placebo (1299 participants)
- Three trials [8-10] compared Remdesivir with standard of care (6153 participants). Of these, one trial [8] had two arms with different durations of Remdesivir (5 days arm and 10 days arm) compared with a standard of care arm (596 participants).
Our expert working group classified progression to oxygen, non-invasive ventilation (NIV) and invasive mechanical ventilation (IMV) as critical outcomes and mortality, time to clinical improvement and thrombotic or secondary infections as important outcomes. However, as the situation in the country evolved, the guidelines group upgraded mortality, time to clinical recovery and time to clinical improvement as critical outcomes, as an effect on those could reduce pressure on the overwhelmed health system.
Critical (primary) Outcomes
As presented in the ‘Summary of findings’ table, the evidence is of low or very low certainty about the effect of Remdesivir on mortality, progression to non-invasive ventilation or high flow oxygen, progression to invasive mechanical ventilation, time to clinical recovery (not requiring oxygen or hospitalised care) and adverse events leading to drug discontinuation.
(a) All-cause mortality: Low certainty of evidence in 7400 patients in five RCTs [7-11] found little or no difference between Remdesivir and placebo or standard of care (RR 0.94; 95% CI 0.82 to 1.07).There were no significant differences observed even when trials were stratified by severity, risk of bias or steroid usage.
(b) Time to clinical recovery (time to achieve WHO score 1,2,3 or not requiring hospitalization for oxygen or medical care): In 1459 patients from two RCTs [8;11], the hazard ratio (HR) for reduction of time to clinical recovery in participants receiving Remdesivir compared with those receiving placebo or standard of care was 1.22 (95% CI 1.06 to 1.41). The evidence was of very low certainty. The median time reported in two studies ranged from 6-10 days in the Remdesivir group vs 7-15 days in the control groups (See Results Table 1 for results from each trial). A mean difference to quantify the magnitude of potential benefit was not available.
(c) Time to clinical improvement (>2 point reduction in the WHO ordinal score): Low certainty evidence from 1688 participants in three RCTs [7;8;11] suggested that Remdesivir may decrease time to clinical improvement (HR 1.25; 95% CI 1.12 to 1.40). The median and IQR ranged from 6-21 days in the Remdesivir group vs. 6-23 days in the control group. (See Results Table 1 for results from each trial). A mean difference to quantify the magnitude of potential benefit was not available.
(d) Progression to oxygen therapy: Low certainty evidence in 138 patients from one RCT [11], found that Remdesivir may make little or no difference in progression to oxygen therapy vs. standard of care (SOC)/placebo (RR 0.81; 95% CI 0.54 to 1.22).
(e) Progression to non-invasive ventilation (NIV) or high flow oxygen (HFO): Evidence from 573 patients in one RCT [11] found that Remdesivir may reduce progression to NIV or HFO (RR 0.70; 95% CI 0.51 to 0.98) and varied as widely as 2% to 49% with small sample size and few events.
(f) Progression to invasive mechanical ventilation: The evidence from 5730 patients in two RCTs [9;11] found that the effect of Remdesivir on progression to invasive mechanical ventilation was very uncertain (RR 0.78; 95% CI 0.44 to 1.39).
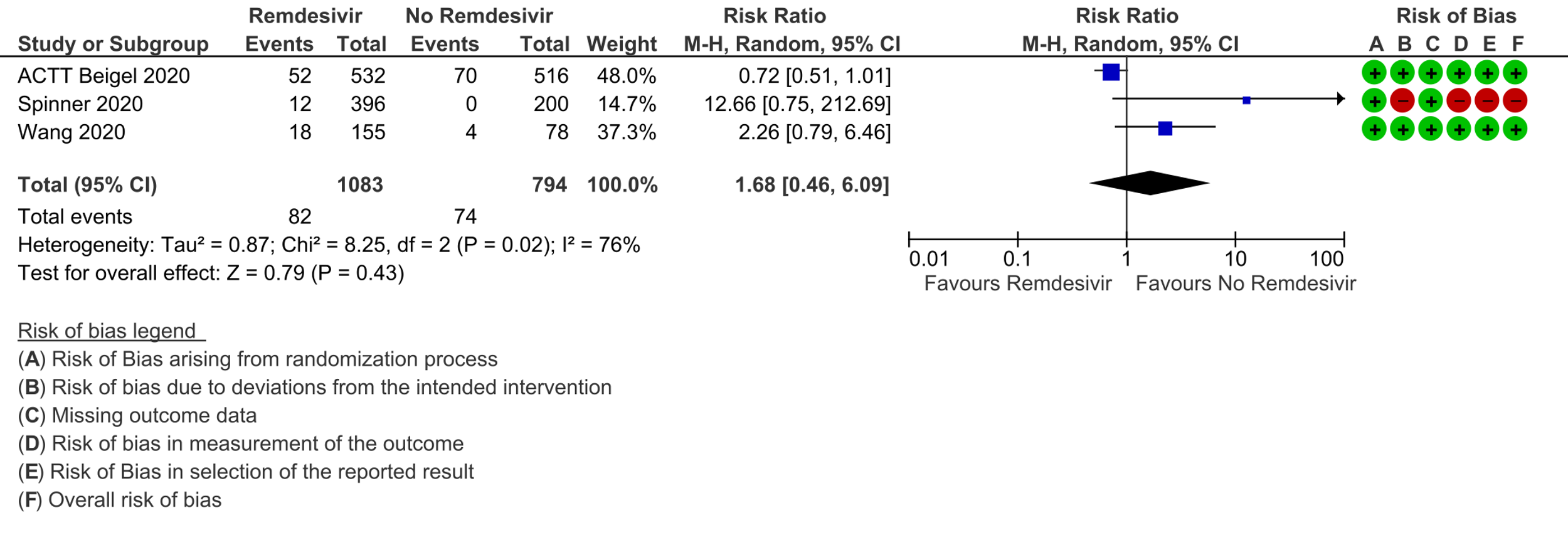
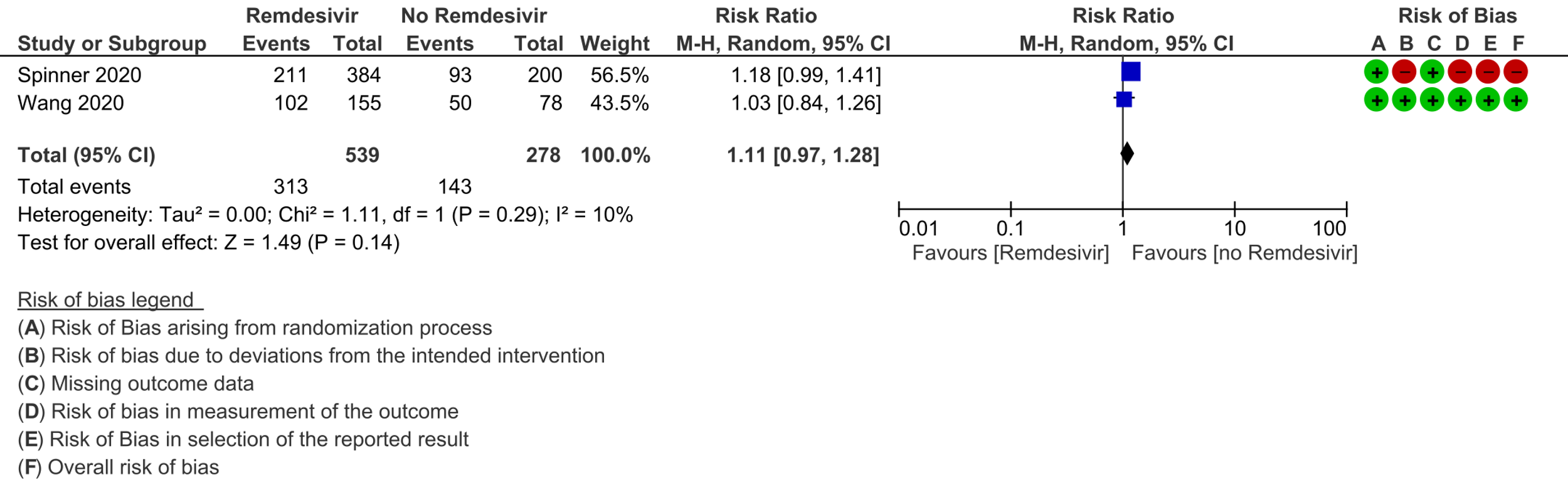
(g) Adverse events: Low certainty evidence from 817 patients in two RCTs [7;8] revealed Remdesivir may contribute to few or no additional adverse events as compared to placebo (RR 1.11; 95% CI 0.97 to 1.28). In addition, very low certainty evidence from 1877 patients in three RCTs [7;8;11] were found regarding the effects of Remdesivir on adverse effects leading to drug discontinuation (RR1.68; 95% CI 0.46 to 6.09).
(h) Duration of hospitalization: This was reported in two studies as a median and hence a meta-analysis could not be performed. Wang 2020 [7] reported a median (IQR) of 21 (12 to 31) days in the Remdesivir group vs. 21 (13.5 to 28.5) days in the SOC or placebo groups. ACTT Beigel 2020 [11] reported median (IQR) as 12 (6-28) days vs. 17 (8-28) days in the SOC/placebo groups.
Important (secondary) outcomes:
(1) Thrombotic events: Low certainty evidence from two RCTs [7;11] in 1281 participants suggests that Remdesivir may make little or no difference to occurrence of thrombotic events when compared to placebo or SOC (RR 0.74; 95% CI 0.40 to 1.37).
(2) Secondary infections: Low certainty evidence from two RCTs [7;11] in 1281 participants suggests that Remdesivir make little or no difference to occurrence of secondary infections when compared to placebo or SOC (RR 0.44; 95% CI 0.16 to 1.18).
No comparative data could be extracted for time to negative PCR; or post-acute COVID-19 pulmonary function/fibrosis or other sequelae.
Subgroup analysis
A subgroup analysis was attempted as pre-specified by the Expert Working Group.
- In two RCTs [7;9] with 1,463 participants, in the subgroup with pneumonia but no hypoxia Remdesivir did not show a mortality benefit (RR 0.85; 95% CI 0.42 to 1.72).
- In one RCT [7] Remdesivir showed no mortality benefit when participants were stratified by shorter duration of symptoms (<10 days; RR 0.76; 95% CI 0.29 to 1.95) or ≥10 days of symptoms (RR 1.48; 95% CI 0.45 to 4.88).
Disaggregated data could not be obtained for co-morbidities, inflammatory markers or different age groups. Subgroups of pregnancy, lactation, renal failure, liver failure were excluded from most trials. No data were available separately for immunocompromised individuals in any of the trials.
Results Table 1: Time to clinical improvement and recovery
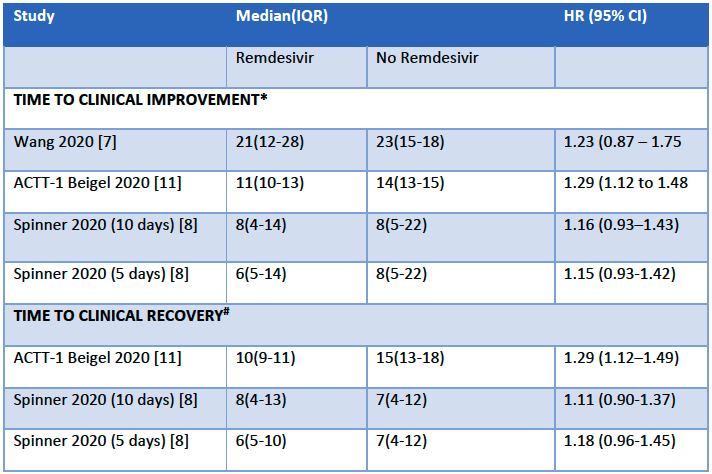
*Time to clinical improvement was defined as the time to a two-point reduction in patients’ admission status on a six-point ordinal scale
#Time to clinical recovery was defined as the time to being non-hospitalized, or hospitalized with no oxygen or medical care requirement
| Study | Intervention | Design | Location; | Age, | No | Participant |
|---|---|---|---|---|---|---|
| ACTT | Remdesivir (200 mg loading dose on | Double | USA, | Remdesivir: 58.6 Placebo: | Remdesivir: 541 Placebo: | Patients ≥18 years |
| Mahajan | Remdesivir 5 days (200 mg on day 1, 100 four | Open | India; | Remdesivir: 58.08 SOC: | Remdesivir: 10 SOC: | Patients All in the study had radiographic evidence of |
| Solidarity | Remdesivir (200 mg on day 0 and 100 | Open | Worldwide; Inpatients | Not | Remdesivir: 2750 SOC: | Patients ≥18 years old inpatients with Covid-19 |
| Spinner | Remdesivir 5-day and 10-day course (200 | Open | US, Europe and Asia; Inpatients | Remdesivir 10-day arm: 56 Remdesivir 5-day arm: 58 SOC: | Remdesivir 10-day arm: 197 Remdesivir 5-day arm: 199 SOC: | Patients Hospitalized patients>12 years with |
| Wang | Remdesivir (200 mg on day 1 | Double | China; | Remdesivir: 66·0 Placebo: | Remdesivir: 158 Placebo: | Patients ≥18 |
1. Mortality, all-cause: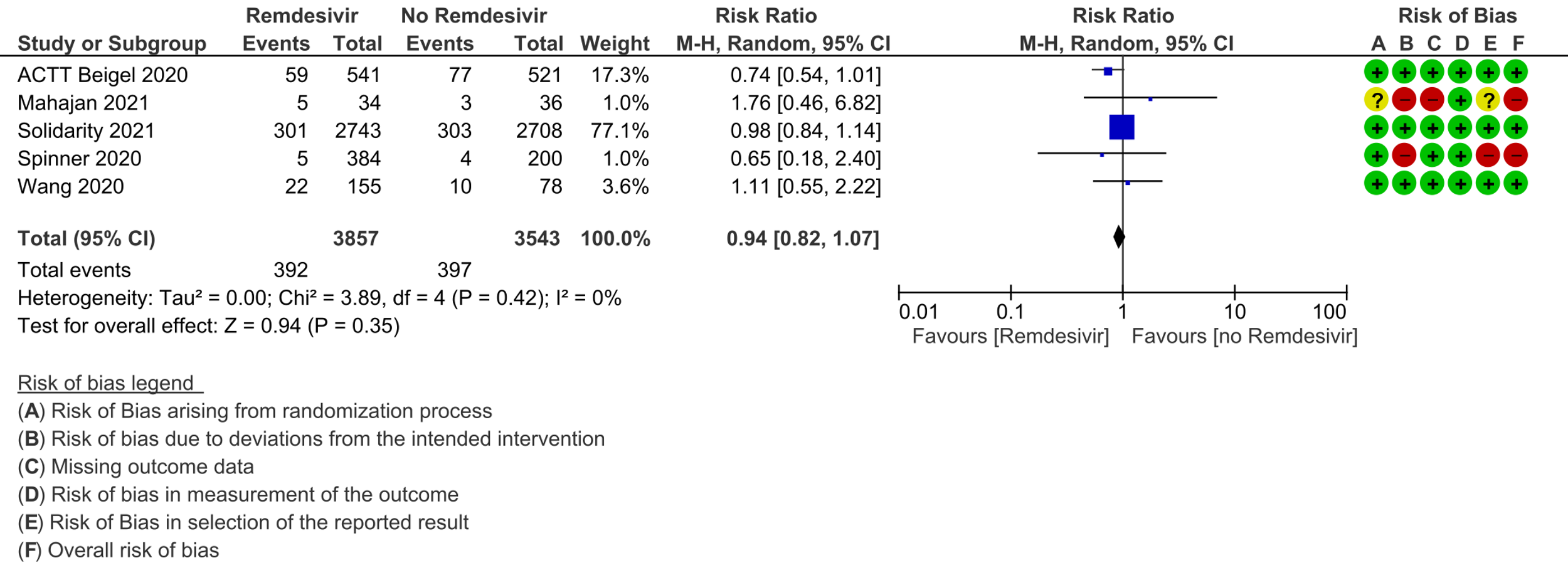
2. Time to clinical recovery:
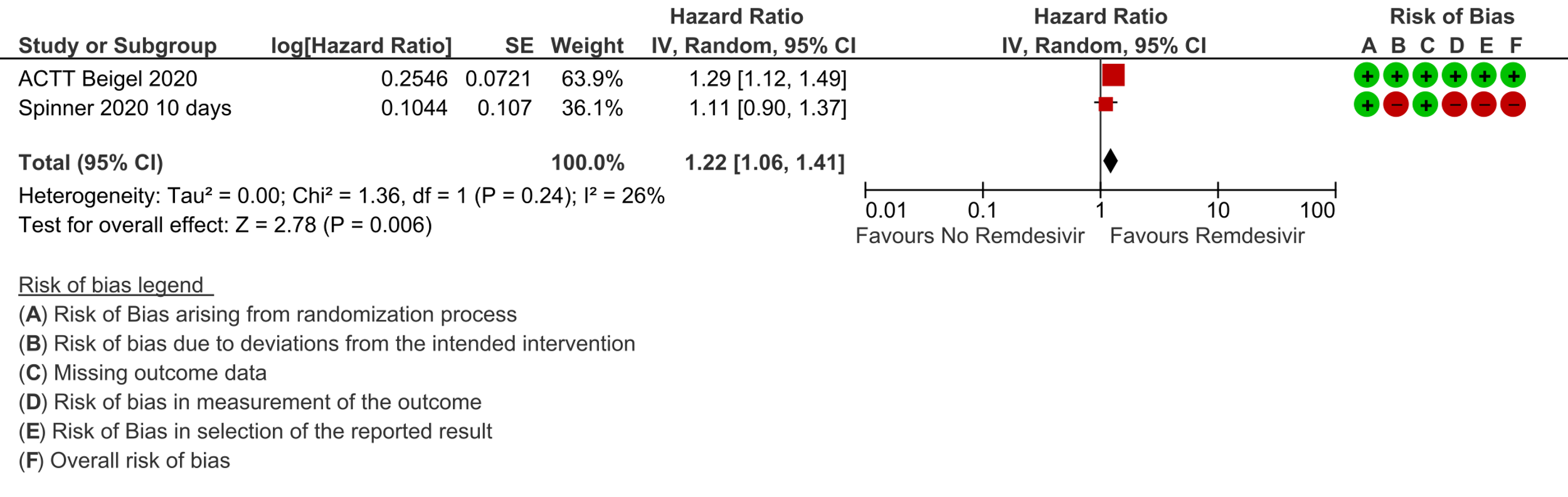
3. Time to clinical improvement:
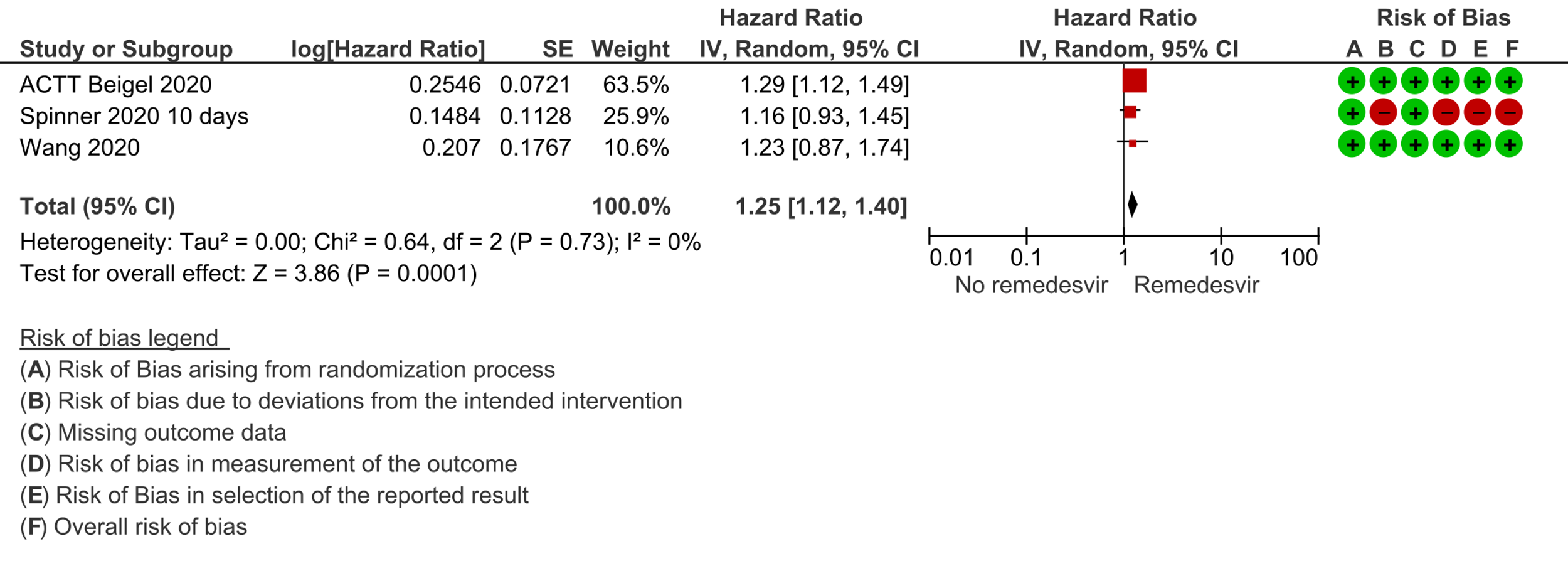
4. Progression to oxygen therapy / 5. Progression to non-invasive ventilation/high-flow oxygen / 6. Progression to invasive mechnical ventilation:
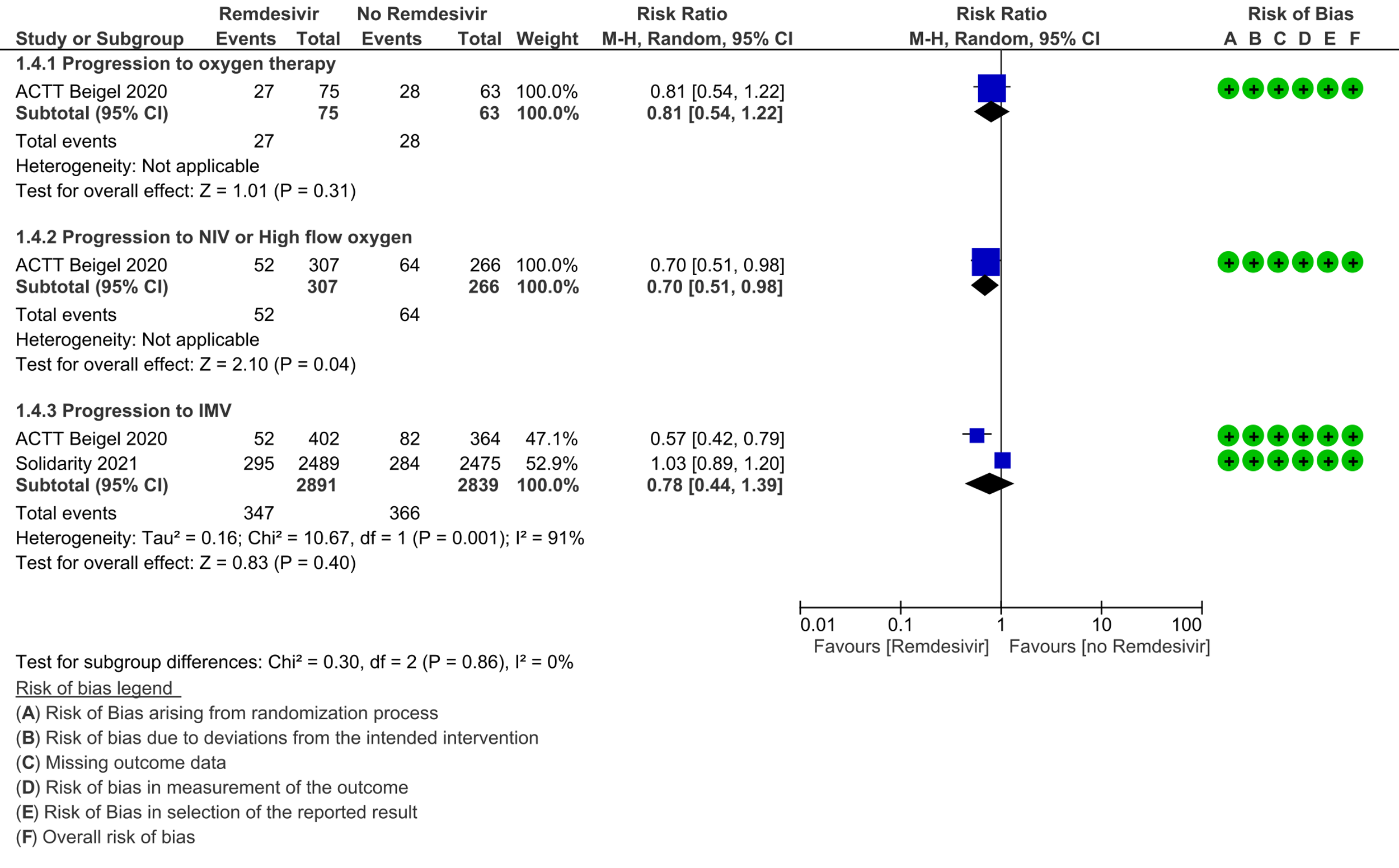
7. Complications: thrombotic events / 8. Complications: secondary infections:

9. Any adverse events:
10. Adverse drug reactions leading to drug discontinuation: